What Are Behavioral Health Services?
Behavioral health treatments are ways of helping people with mental illnesses or substance use disorders. For example, counseling and more specialized psychotherapies seek to change behaviors, thoughts, emotions, and how people see and understand situations. Medications for mental and substance use disorders provide significant relief for many people and help manage symptoms to the point where people can use other strategies to pursue recovery. For many people, the most effective behavioral health approach involves a combination of counseling and medication. So, let’s find out what are behavioral health services.

Behavioral Health Versus Mental Health
Behavioral health describes the connection between the health and well-being of the body and the mind. This can include a variety of areas – everything from eating habits to drinking habits to exercise and various mental health challenges. Behavioral health can extend to psychiatric conditions, marriage and family counseling, and addiction treatments. For every 10 people who visit a doctor, there are seven who are there for reasons related to behavioral health, according to the Maine Health Access Foundation. But what is behavioral health, and how does it impact the lives of employees?
The terms “behavioral health” and “mental health” are often used interchangeably, but there are some distinct differences. The best way to think about it is that mental health is just one aspect of the larger category of behavioral health. For example, an employee might need to tap into behavioral health benefits, but what they might specifically need is help to manage depression or help with a substance abuse issue.
The term “behavioral health” may also have less of a stigma, which may encourage people to reach out and get help when they need it. The services and options available to a person seeking help are also more diverse, giving them resources that weren’t available in the past to resolve their challenges.
A Breakdown of Behavioral Health Services
The variety of services available to employees who need help has expanded in recent years. These services are targeted to help people live healthier lives in regard to their mind, body, and overall health. There are a variety of services that a person might need depending on his or her individual challenges. One person may need help with substance abuse, while another may be managing bipolar disorder – and another might need help with marital problems.
The services are targeted to assist with a variety of issues – everything from depression to anxiety to diabetes management, weight loss, drinking, and drug use and much more. The issue a person is facing will determine which type of healthcare provider and service is most relevant. Examples of services that an employee can tap into through a behavioral health program include the following.
Behavioral Health Services: Psychiatrists
These providers can help with a variety of challenges, from child and adolescent psychiatric issues to geriatric psychiatry to addiction psychiatry. In addition, these providers can write prescriptions to assist with the healing process if the patient’s condition is required.
Behavioral Health Services: Psychologists
These providers are trained in the science of psychology and work in a clinical, counseling, or research setting. They work to diagnose and offer psychotherapy to assist with healing the patient’s condition.
Behavioral Health Services: Social Workers
These professionals can provide a wide variety of services, usually in administrative positions within programs and institutions to assist people. For example, there are medical and health social workers, child, family, and school social workers, and mental health and substance abuse social workers, just to name a few areas in which these individuals work.
Behavioral Health Services: Licensed Professional Counselors
These counselors typically specialize in psychotherapy to assist with a patient’s condition. These professionals may focus on specific behavioral health areas, such as marriage issues or substance abuse. LPCs typically don’t provide a formal diagnosis or prescribe medications.
Behavioral health services are designed to treat the underlying cause(s) of a specific behavior. For example, in the field of suicide prevention, the practitioner won’t only want to prevent the behaviors that may result in suicide but also to understand the underlying causes of those behaviors to help the patient in the long term.
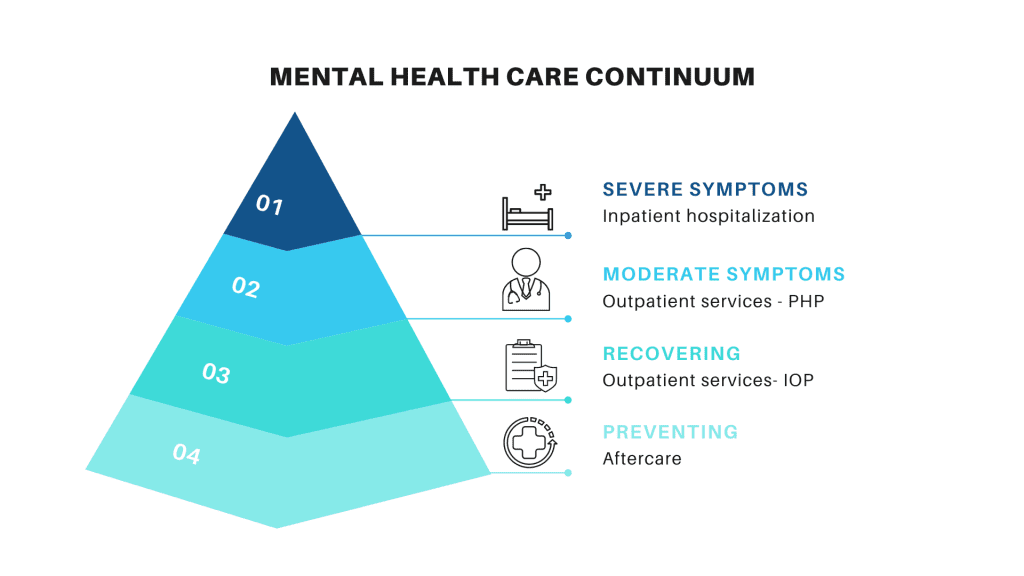
Common symptoms of mental health/ behavioral health issues
Common symptoms of a potential mental health issue or behavioral health issue include but are not limited to:
- Feeling sadness or overwhelming depression.
- Exhibiting a reduced ability to concentrate.
- Worrying excessively or experiencing unnecessary fears.
- Exhibiting extreme mood swings or emotional changes.
- Withdrawal from activities, friendships, and other social gatherings.
- Significant changes in eating habits.
- Suicidal thoughts or active thinking about harming yourself or others.
- Signs of dementia or lack of intellectual ability (especially those over the age of 55).
- Substance abuse.
Increased levels of stress, fear, and distress can be linked to behavioral health issues through the influence of the immune and cardiac functions of the body. If any/all of these signs or symptoms are actively present, seek the guidance of a primary care provider, behavioral health counselor, or mental health professional.
- Mental illness impacts millions of American lives; however, many live without knowing that they can receive treatment or care for their conditions.
- Behavioral health is a vast field, meaning forms of treatment or behavioral health care can look different for each patient depending on what they need help with.
- It’s common for the term ”behavioral health” and ”mental health” to be used interchangeably despite their distinct differences.
- When thinking about behavioral health in terms of insurance, it can be challenging to understand what is covered.
Behavioral health services focus on daily habits, behaviors, and actions that can impact a patient’s mental and/or physical health. For example, when examining the behavioral health needs of a patient, a behavioral health provider may look at the patient’s daily exercise or eating habits to see how they are linked to their levels of anxiety or depression. Many in the medical field view behavioral healthcare as more holistic, calling it ”better care and health for the whole person.”
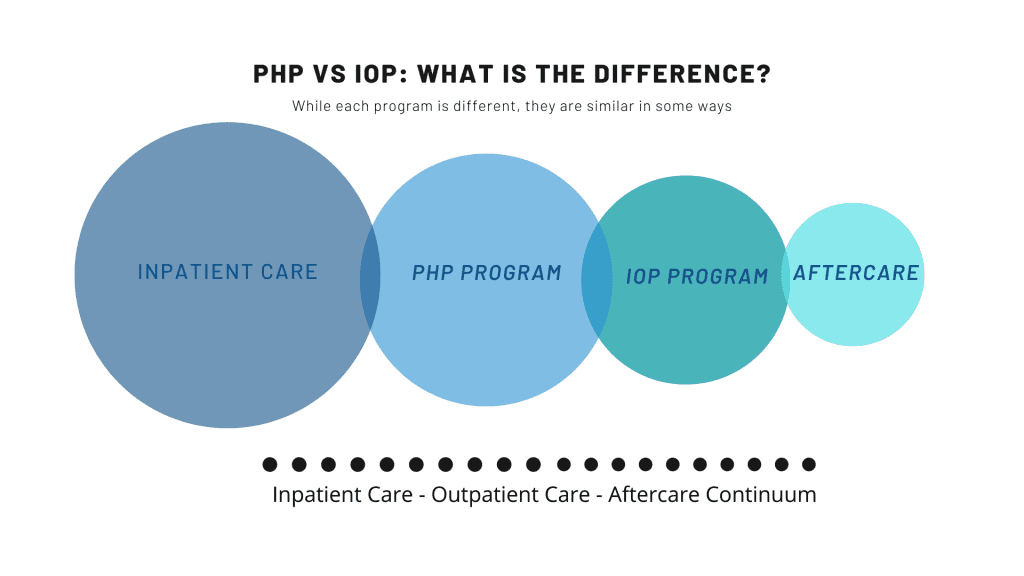
Understanding the impact of behavioral health
Recent studies have shown that over 44 million Americans are currently suffering from mental illness; however, only 43% are actively receiving care. In the same vein, almost 20 million Americans suffer from substance abuse disorders; meanwhile, only 11% are receiving care. To put that into perspective, 44 million suffering from a mental illness is greater than the entire population of California; 20 million suffering from substance abuse disorders is equivalent to the entire population of Florida. Furthermore, when looking at those Americans, ”Up to one-third of adults potentially meet the criteria for a past year behavioral health disorder,” with ”half report[ing] that their disorders were first experienced by age 14, and almost three-quarters report[ing] that their disorders were first experienced by age 24.” Behavioral healthcare affects people across the nation, with ages ranging from an infant to an older adult 55 and up. Studies show that 20% of people over the age of 55 suffer from a mental disorder, with two-thirds of nursing home residents exhibiting behavioral health problems. However, only 3% of those reported adults are actively seeing a mental health professional for their symptoms and disorders. This shows that the disorders the behavioral health field handles touch the lives of many, yet the majority affected don’t recognize they are suffering or know that they have access to care.
Behavioral health counseling and treatment
When looking into treatment for a behavioral disorder, a patient will find that a behavioral health professional and their services are more common than believed. For example, a social worker, counselor, psychiatric nurse practitioner, neurologist, and even a primary care provider are all linked to and trained to administer forms of treatment for a behavioral disorder. Furthermore, treatment programs can be facilitated in numerous ways depending on the behavioral health issue or mental disorder the patient may have e.g. inpatient programs, outpatient programs, specialized rehabilitation programs, therapeutic programs such as cognitive behavioral therapy, etc.
Once the client picks their trusted behavioral health consultant, their first behavioral health consultation may consist of the doctor examining or asking questions to the patient about a wide range of ”behaviors” and prior medical history. For example, it is common to assess if the patient is struggling with a present or past substance abuse disorder, a relationship with gambling or other addictive behaviors, their life at school or at home, their history of trauma, or struggle with a past health condition, different components of their mental health including past diagnoses of a mental health issue, their relationship with food or exercise in case of the presence of an eating disorder, etc. Fundamentally, behavioral health requires a vast look into a patient’s background because their daily routine involves a variety of components that can have a significant effect on their mental and/or physical health. Symptoms are often complexly interconnected and vary from patient to patient.
Behavioral health and insurance: What is covered?
What many people don’t know is that in 2008 the Paul Wellstone and Pete Domenici Mental Health Parity and Addiction Equity Act was created, often called the ”mental health parity law” or the ”federal parity law.” The American Psychological Association stated that this law ”requires insurance companies to treat mental health and behavioral health and substance use disorder coverage equal to (or better than) medical/surgical coverage.” Two big areas of insurance that were affected were co-pays and visit limitations. One example of this is, if an insurance company only requires a $20 co-pay for most medical visits then they must issue the same co-pay for a mental/behavioral health visit. In regards to visiting limitations, it used to be common for insurance companies to place a limit on the number of mental health visits a client could have in a year; however, this is no longer allowed.
Despite this law, there are still a few setbacks, such as:
- Insurance companies can still place a ”medical necessity” limit on mental health, behavioral health, and substance disorder visitations.
- Psychologists and other behavioral service providers have the discretion over which insurance plans they accept.
- The parity law does not require insurers to provide behavioral health benefits; it just requires that if they do, they can’t have more restrictive requirements than physical/medical health benefits.
However, when looking at insurance plans, the parity law does actively affect:
- Employer-sponsored health coverage for companies with 50 or more employees.
- Coverage purchased through health insurance exchanges that were created under the healthcare reform law, also known as the Affordable Care Act or ”Obamacare.”
- Children’s Health Insurance Program (CHIP).
- Most Medicaid programs.
When looking at health insurance coverage, it’s essential to check the plan’s benefits description to ensure behavioral health, mental health, and substance disorder visitations are covered. If it’s unclear, speak directly to the insurance company for more details.
Checking an insurance plan’s benefits.
Due to the California Mental Health Service Act (MHSA), most health insurance plans, offer coverage for behavioral health care or mental health care. When struggling to figure out what an insurance plan covers regarding doctors, clinics, prescriptions, etc. be sure to log onto the insurance company’s online platform and check the ”Summary of Benefits and Coverage” section, often called an ”SBC.” It is required for all insurance companies to have this document, which outlines all of the services and benefits it provides. If it’s still unclear, contact the company directly via phone or email to get more information.
If your insurance does not cover mental health, consider using other financing options.


At Overland Intensive Outpatient, our philosophy is to help treat mental health by uncovering the underlying causes and addressing the co-occurring disorders which could drive the individual to relapse. We understand that every person who enters our doors comes with unique needs and goals. Our experienced clinicians will work one-on-one with clients to develop a comprehensive treatment plan using evidence-based methods. Overland Intensive Outpatient is ready to provide both in-person and virtual care (telehealth services) to expand access to essential health services and meet the health needs of our patients.
If you need FREE help please contact the National Helpline about mental and/or substance use disorders, prevention, treatment, and recovery in English and Spanish.
Published: April 03, 2022
Last Updated: July 09, 2025

Published: May 01, 2026
IOP for Substance Abuse and Co-Occurring Disorders in Los Angeles, California
Substance use disorders do not develop in a vacuum. Behind nearly every addiction, whether to alcohol, opioids, benzodiazepines, methamphetamine, cocaine, or prescription medications, there is an underlying mental health condition that either precipitated the substance use, emerged alongside it, or was worsened by it. According to the National Institute on Drug Abuse, approximately half of […]
Read more
Published: April 11, 2026
IOP for OCD in Los Angeles, California
Obsessive-compulsive disorder affects approximately 2.5 million adults in the United States, yet it is one of the most misunderstood and undertreated mental health conditions. People with OCD experience intrusive, unwanted thoughts (obsessions) that produce intense anxiety, followed by repetitive behaviors or mental rituals (compulsions) performed to reduce that anxiety. The cycle is self-reinforcing: compulsions provide […]
Read more
Published: April 01, 2026
IOP for Bipolar Disorder in Los Angeles, California
Bipolar disorder affects approximately 4.4% of U.S. adults at some point in their lives, according to the National Institute of Mental Health. It is one of the most complex mood disorders to treat because it involves cycling between distinct emotional states (depressive episodes, manic or hypomanic episodes, and mixed episodes) each requiring different clinical approaches. […]
Read more
